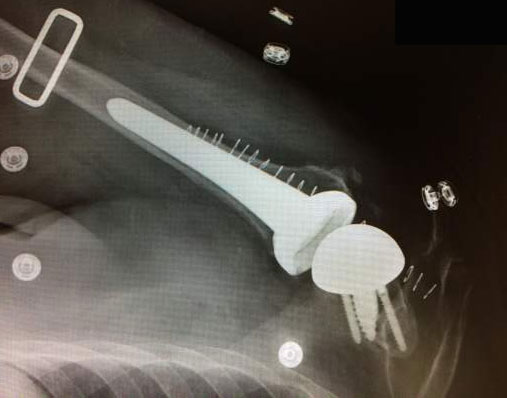
Dr. Richard Steinfeld offers a unique service to his joint replacement surgery patients. Following surgery, each joint replacement patient will have a dedicated medical staff member from the practice visit them at their house during their recovery to ensure all of their post-operative medical needs are attended to. Our Patient Care Liaison, Nicki Harrelson, MA, has greater than 20 years of experience caring for post-op joint replacement patients.
In addition, a dedicated phone number is supplied to the patient to contact the staff member directly at any time during their recovery period. This gives the patient direct access to the surgeon in time of need. Our joint replacement patients can now be reassured of their progress, have their questions/concerns addressed directly, avoid confusion or misinformation during their recovery, and potentially avoid unnecessary ER or Urgent Care visits. The Orthopaedic Center of Vero Beach is proud to offer this unique service to our joint replacement patients.





 This year the
This year the